How Topology Optimization Could Be the Key to Longer-Lasting Hip Implants
Hip stem implants must support the mechanical loads of the patient’s lifestyle, but should also avoid stress shielding. A team from Altair leveraged simulation, topology optimization and 3D printing to design an optimized hip stem that meets both conditions.
Conventional implants used in total hip replacement surgeries are generally expected to last about 20 years, on the assumption that the patient will mostly use the hip during light activity like standing and walking. But increasingly, patients demand much more from their hip implants. Hip replacement candidates today are trending younger and tend to be more active with lifestyles that include biking, swimming, jogging and even mountain climbing. Providing implants to these unconventional patients requires an unconventional design and manufacturing approach.
Additive manufacturing (AM) can help. Metal 3D printing has been used to make titanium implants for at least the last decade, and offers the ability to customize the size and shape of an implant as well as its stiffness, porosity and other attributes. 3D-printed implants incorporate lattices and textures that allow for better bone in-growth, helping patients heal faster and ensuring that implants are secure over the long term.
But AM also offers another potential benefit for hip implants: the ability to customize the implant for the specific loads it is expected to bear. In combination with topology optimization, additive manufacturing makes it possible to create better-fitting, longer-lasting and higher-performing hip implants for the specific patient. A recent case study from Altair leveraged the company’s simulation tools to create a methodology for designing hip stem implants putting these ideas into practice.
Simulation As a Design Tool
A team from Altair consisting of Yuhao He, Drew Burkhalter, David Durocher and Mak J. Gilbert applied the company’s software to develop an improved hip stem implant and presented their findings at the 2018 Design of Medical Devices Conference. The 3D-printed hip stem they created was designed using the principles of topology optimization—that is, a design approach that defines an overall design space and then fills it strategically to meet the load, weight and other requirements for the part. When paired with the manufacturing capabilities of 3D printing, topology-optimized parts often feature organic shapes and lattices rather than straight lines and solid forms. These parts are often lighter than their conventional counterparts as a result of this strategic material usage.
But to ensure that these final topology optimized parts will meet performance needs requires the ability to first define what those needs are. Altair’s answer to this need is a package of tools within its Inspire software suite for simulating parts under expected loading conditions, alone or as part of an assembly. Users can see how a given geometry and material will interface with its surroundings and stand up to expected usage, gathering information that can then inform the topology optimization. The software allows the user to simulate an existing part to gather load data, for example, and then feeding subsequent design iteration back into the simulation to see how changes affect performance. This recursive process enables engineers to use simulation not just for testing final designs, but as a design tool itself.
Topology Optimizing a Hip Stem
In redesigning a conventional hip stem implant, Altair’s engineers set out to create an alternative that would achieve two things. First, the implant needed to support the mechanical loads required by a patient’s body and lifestyle over time. But it also needed to meet biocompatibility requirements to ensure a secure interface with the patient’s bone while minimizing stress shielding, a condition where the bone density is reduced from a decrease in bone stresses caused by an implant. The best-case scenario hits on the right combination of sufficient strength but limited stiffness that mimics the natural bone.
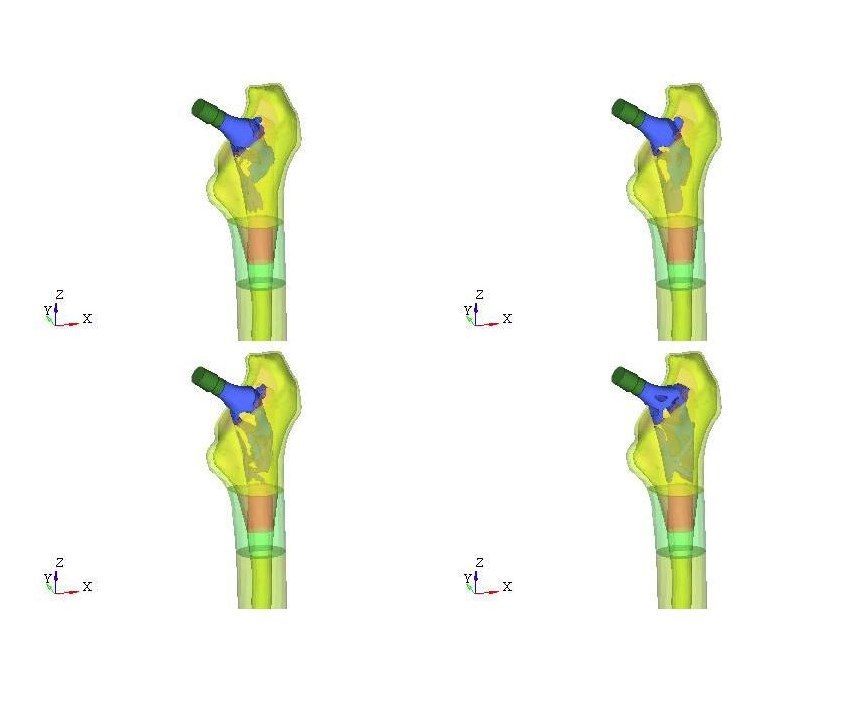
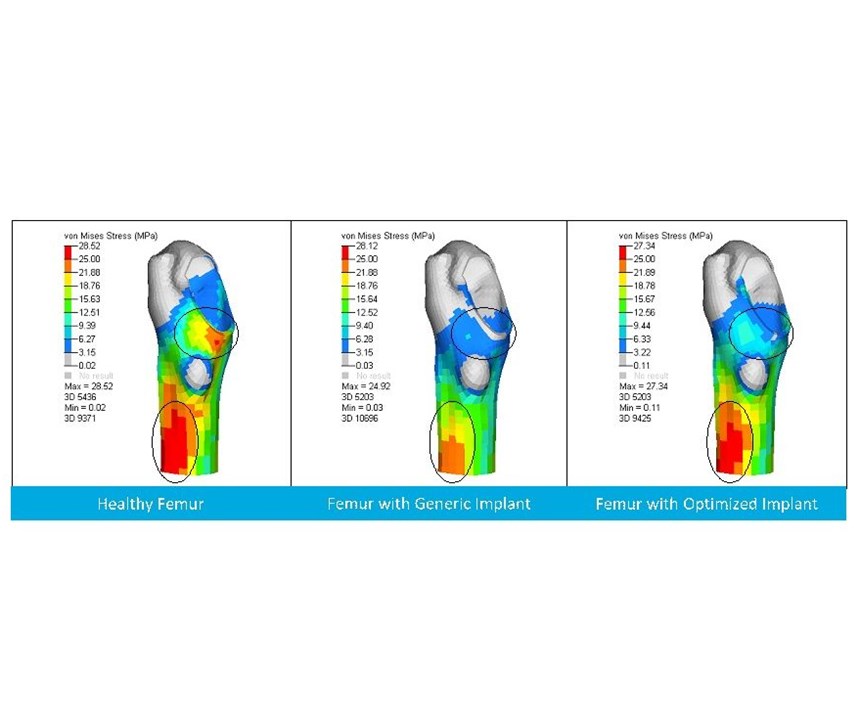
For the case study, the team elected to design a hip stem’s neck that would support loads required for standing up from a sitting position, standing, climbing stairs and jogging, as well as a combined load case. The team simulated how a healthy femur and a femur with a generic titanium implant would behave under these loading conditions, looking at changes in stress distribution, strain energy and stress shielding. This data helped to inform an optimized design that distributes stress and strain more like natural bone, and reduces stress shielding over a generic implant.
The topology-optimized implant was designed using the generic implant as the design space to ensure that the resulting hip stem would fit a human femur and be compatible with current surgical tools. The team also placed constraints on the design software to control strain distribution and the volume fraction, restricting the latter to less than or equal to a 10, 20 or 30 percent departure from the generic volume in various tests. Finally, design possibilities were limited to those that could be 3D printed in titanium using selective laser melting (SLM) in a machine from EOS.
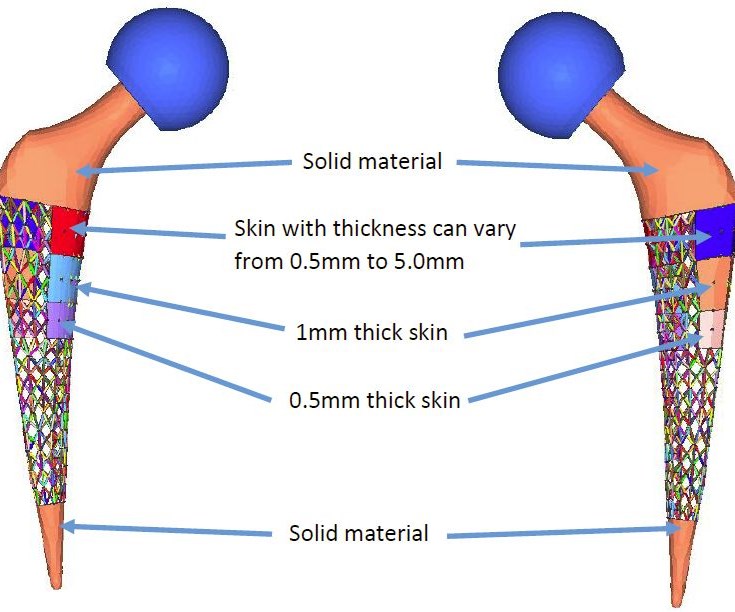
The topology optimization results determined the solid and semi-dense areas of the implant, and the team then used Altair OptiStruct to fill the semi-dense regions with lattice. The lattices were constrained to meet fatigue strength requirements while minimizing total volume to speed manufacturing.
The unit cell selected for the lattice features beams that follow the four vertical edges of a cube, with the eight corners connected with face centers and body center. Because the implant was intended to be printed in the vertical direction, the overhang angle for the lattice beams is less than 45 degrees to enable 3D printing without the need for support structures. The cell size ranges from 4 to 7 mm; lattice optimization helped to determine the optimal diameter of each lattice beam and ligament.
The final implant design features solid material for the hip stem’s neck and bottom tip, where bone in-growth could cause pain for the patient. A variable lattice fills the middle section, with a skin on the medial side to help meet fatigue requirements.
The team then fed the topology optimized implant design back through the load case simulations to compare its performance versus an intact femur and femur with a generic implant. They found that stress shielding was reduced for the optimized implant over the generic one for all load cases. The optimized implant offered a stress shielding reduction of 50.7 percent averaged over all five load cases. Stresses in the stem remained below 575 MPa for all load cases; for the titanium grade used in the study, this would mean an endurance limit of about 10 million cycles.
In the short term, this simulation-driven methodology for implant design could help to reduce stress shielding in universal or standard medical implants. But over the long term, customized implants could be designed using this method, tailored to the patient’s femur geometry and bone characteristics as well as his or her lifestyle. And given 3D printing as the production method, these individualized implants might even be made about as quickly and as cost-effectively as if they were standard implants.
Related Content
Stratasys, CollPlant Unite Technologies for Industrial-Scale Bioprinting of Tissues, Organs
The joint development and commercialization agreement will initially focus on development of a bioprinting solution for CollPlant’s regenerative breast implants, addressing $2.6 billion market opportunity.
Read MoreMore Affordable Suture Anchors 3D Printed from PEKK: The Cool Parts Show #60
Selective laser sintering (SLS) of polyether ketone ketone (PEKK) is being used to produce medical implants that are more cost effective and perform better than their conventional counterparts. We highlight fasteners known as suture anchors in this episode of The Cool Parts Show.
Read MoreNew Zeda Additive Manufacturing Factory in Ohio Will Serve Medical, Military and Aerospace Production
Site providing laser powder bed fusion as well as machining and other postprocessing will open in late 2023, and will employ over 100. Chief technology officer Greg Morris sees economic and personnel advantages of serving different markets from a single AM facility.
Read MoreMSU, AddiTec Collaborate to Develop Biocompatible Bone Implants
The collaboration focuses on enhancing Ti-6Al-4V implant properties by incorporating alloying elements such as Tricalcium phosphate to the Ti-6Al-4V melt pool matrix — which cannot be done conventionally.
Read MoreRead Next
3D Printed Hips Versus the World's Deadliest Mountain
3D printed trabecular titanium hip implants—printed by Lima Corporate on Arcam EBM machines—helped legendary Italian mountaineer Romano Benet to continue scaling the world's most dangerous peaks.
Read MoreAt General Atomics, Do Unmanned Aerial Systems Reveal the Future of Aircraft Manufacturing?
The maker of the Predator and SkyGuardian remote aircraft can implement additive manufacturing more rapidly and widely than the makers of other types of planes. The role of 3D printing in current and future UAS components hints at how far AM can go to save cost and time in aircraft production and design.
Read More3D Printing Brings Sustainability, Accessibility to Glass Manufacturing
Australian startup Maple Glass Printing has developed a process for extruding glass into artwork, lab implements and architectural elements. Along the way, the company has also found more efficient ways of recycling this material.
Read More
.jpg;width=70;height=70;mode=crop)