Leveraging Additive Manufacturing to Improve Joint Replacement Surgery
A German medical device company has turned to metal additive manufacturing to manufacture its acetabular cup cutter for hip and knee replacement surgeries. The cutter’s 3D-printed blades are more reliable and cost-effective, and have improved the surgical experience for both patient and physician.
Revision of a failed acetabular hip implant (the cup-shaped socket in the hipbone that receives the head of the thighbone) is one of the most challenging aspects of revision hip arthroplasty. Implant removal is a time-consuming, yet necessary, step during revision hip replacement surgeries. Because of the diversity of the cups and the methods used to secure them, an equal diversity of approaches and tools are necessary for removal.
Many revision instruments are available for removing the acetabular component of a hip replacement, including chisels, ultrasound tools and commercially available purpose-built devices, such as the endoCupcut acetabular cup cutter from Germany-based medical company Endocon.
Founded in 1998, Endocon develops artificial joint replacement and reusable surgical instruments. In close cooperation with users and partner companies, the company develops , designs and produces products using the latest manufacturing technologies exclusively in Germany.
To avoid the use of a chisel to remove the hip cups during revision—which risks damaging bone and tissue and can leave an uneven surface, making reinserting a new implant difficult—Endocon has created an acetabular cup cutter. This innovative device features additively manufactured cup-shaped blades, which reduces time in surgery and addresses both patient safety and experience.
“The endoCupcut allows for more precise cutting along the edge of the acetabular cup, and gives surgeons the opportunity to loosen and extract cementless hip cups quickly, without adding additional damage to the surrounding bone,” says Klaus Notarbartolo, general manager at Endocon. “While some other suppliers’ cup cutters are single-use or are made out of one piece (the cutting blades are fixed to the handle), they are more expensive than our system, which is reusable and allows surgeons to implant the same size hip cup that was implanted before. It offers variability in one instrument and can be combined with up to fifteen additively manufactured stainless steel blades, in various shapes and sizes, ranging from 44 to 72 mm.”
Alternative to Traditional Casting Needed
Traditionally, the cutting blades for this surgical tool have been manufactured using traditional casting. However, this manufacturing method represented a few disadvantages for the surgeon as well as for Endocon as a manufacturer.
Production time. Relying on a time-consuming, laborious method like casting, especially for multiple sizes and shapes, meant that the production time for a single batch of blades could be as long as three and a half months. That made it necessary to keep blades in stock, which of course is expensive.
Quality. Casted blades often present other problems, such as corrosion, quality challenges and difficulty achieving consistent hardness without reducing tensile strength, resulting in a rejection rate of around 30 percent. Hardness is important for this tool, as it has to withstand enormous forces. Since the hardness was not always easy to determine due to the complex geometry of the blades, blades could break during surgery, Notarbartolo says. Moreover, hardness testing had to be destructive, requiring an additional set of blades to be manufactured just for testing purposes.
Complex design process. Due to the solidification process after casting, the complex-shaped knives exhibited deflections that had to be compensated for in the CAD data. This compensation had to be done for every single blade, in all sizes and short and long versions that exist. Still, there were some batches which exhibited deflections, and no one knew why.
Costs and flexibility. Keeping stock was expensive, but quality problems as explained above drove costs up, as well. Moreover, a tool breakage or a surgeon’s need for an unusual blade size for an extremely small or tall patient meant that Endocon had to be able to deliver an unusual size as soon as possible..
In an effort to find alternative ways to manufacture the blades, Endocon spoke to several service bureaus and machine shops. Trials to use conventional machining technologies, i.e. milling, all failed or resulted in high costs (twice as high as casting), because the freeform surfaces took too long to machine, andgenerated more than 95 percent wasted chips; subsequent tempering after machining generated deflections/deviations similar to the castings.
The Alternative: Metal Additive Manufacturing
The other alternative Endocon was looking at was additive manufacturing. Since 2011 the company had been running trials on SLM machines but the quality was never sufficient for the production of end-use parts. In 2015, Endocon started test runs with the Fraunhofer Institute and talked to Concept Laser to find a way to produce higher-quality cutting blades on the laser melting machines. Concept Laser recommended talking to the service bureau Weber KP Konstruktion & Prototypen in Bretten, Germany. And that’s when the project gained momentum, according to Notarbartolo.
“After only a few weeks Weber delivered 3D-printed parts that were good enough to start fine-tuning. It only took seven months to manufacture all blades in all sizes, simply amazing!” he says.
Without the long-standing experience of metal additive manufacturing expert Martin Weber (who founded his company in 2007), however, the results wouldn’t have been the same, Notarbartolo emphasizes.
“First we thought we could optimize all parameter settings, geometry and part orientation for one blade and then multiply this according to the different sizes,” Weber remembers. “But we were wrong. Material testing revealed different hardness and tensile strength levels depending on the part size. We needed stress-free parts without deformations coming out of the machine.”
No Waste: Support Structures Are Essential
To achieve the desired results, Weber soon found out that each blade needed not only different parameter settings, but also a different orientation in the machine with support structures not only designed to support the part during the build process, but to serve as a temperature control. “We tried to avoid support structures to minimize postprocessing, but when we realized that these are important to control the part temperature and cooling rates, we individually designed and adjusted them for each blade size,” Notarbartolo says.
The blades are produced in 17-4PH stainless steel on a GE Additive Concept Laser Mlab Cusing 100R machine and are available in just three weeks, including postprocessing (heat treatment takes one week). Depending on size and orientation in the build envelope between two and six blades can be built on a 90 by 90 mm build platform.
“We’ve also been able to reduce the cost per blade by around 40 to 45 percent. That means cost savings for us and in turn for our customers. When you combine that with a reduction in product development time, higher efficiency and lower rejection rates, then the business case for additive really becomes attractive,” Notarbartolo says.
Stronger, More Reliable Blades
The additively manufactured blades now exhibit excellent corrosion resistance, and instead of cracking after 600 N, show a plastic deformation after applying 1,800 N. According to Weber, previous issues with achieving a consistent hardness level have also been resolved using additive, with an improvement to 42±2 HRC, compared to 32 HRC using casting. Moreover, cubic density of the parts was improved from 97 percent to 99 or even 100 percent, Weber says.
Harder, stronger, more reliable blades not only perform better in the operating room, they also address patient safety concerns by reducing the risk of breakage and embedding splinters into the tissue. Fatigue is indicated by plastic deformation, which keeps over-used tools out of the operating room.
From the surgeons’ and the hospitals’ perspective the risk of failure is taken out of the surgery, saving the hospital both time and money.
“The device has been positively received and is already being used by a number of medical professionals across Germany,” Notarbartolo says. “So far there have been no reported tool breakages during surgery. Our cooperation with Weber has been outstanding and instead of looking at taking AM expertise in-house, we target a long-term partnership with Weber. There are many products I can imagine to be 3D printed in future, and we want to cooperate with Weber, who have the experience and expertise to evaluate which products are worthwhile to be considered to be additively made. We are very excited about future projects!”
Related Content
AM 101: What Is Hot Isostatic Pressing (HIP)? (Includes Video)
Hot isostatic pressing has long been used for metal castings, but is now being applied as a valuable method for closing porosity in metal 3D printed parts.
Read MoreIt’s HIP to Be Additive: Advancing 3D Printed Metals with Hot Isostatic Pressing
Aalberts Surface Technologies-Accurate Brazing is preparing to serve additive manufacturing tomorrow by proving out HIPing recipes at its Center of Excellence today.
Read MoreAalberts Surface Technologies Forms U.S. Heat Treatment Business Unit
Combining 17 diverse facilities into Aalberts Surface Technologies - HIP|Braze|Heat Treatment makes it one of the largest providers of thermal processing and metal joining technologies in the U.S.
Read MoreElementum 3D’s High-Strength Aluminum Alloy Eliminates Need for Heat Treatment
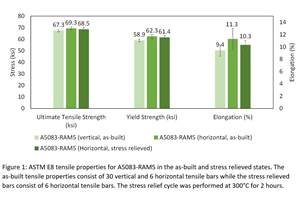
Elementum 3D’s A5083-RAM5 aluminum alloy enables manufacturers to print advanced components from a high-strength aluminum alloy with reduced postprocessing time and cost.
Read MoreRead Next
3D-Printed Metal Device Makes ACL Knee Surgery More Accurate
Additive manufacturing made it possible to produce a medical tool that offers surgeons better control during ACL repair or replacement surgery.
Read More3D-Printed Medical Drills Keep Bone Cool During Surgery
Drills made via additive manufacturing cut bones without causing thermal-induced damage thanks to internal cooling channels.
Read More3D Printing Brings Sustainability, Accessibility to Glass Manufacturing
Australian startup Maple Glass Printing has developed a process for extruding glass into artwork, lab implements and architectural elements. Along the way, the company has also found more efficient ways of recycling this material.
Read More

.JPG;width=700;quality=80)
.png;width=860)
.JPG;width=860)
.JPG;width=860)
.jpg;width=860)