3D Printing Is the Next Step for Digital Dentistry
Digital dentistry is a workflow rather than a single technology. A conversation with Rik Jacobs of 3D Systems explores how 3D printing is participating in and advancing this workflow.

Digital dentistry encompasses a range of technologies including 3D scanning, subtractive milling and, now, 3D printing. Photo: 3D Systems
The challenges include a reliance on skilled labor and its impending loss; problems with accuracy and repeatability; and a multi-step process with many opportunities for things to go wrong. Yet we’re not talking about an aerospace Tier One supplier or a major automaker, nor a mom-and-pop moldmaking or machine shop operation. Instead, the industry facing these challenges is a little more personal: dentistry.
Like other specialized industries, dentistry (including closely related fields like prosthodontics and orthodontics) has been losing the specialist technicians it needs in its workforce — an urgent problem considering just how much manual labor goes into a custom device like a bridge or denture. Each step performed by hand introduces potential pitfalls that require skill and experience to avoid. The final device is a true one-off, with no drawings or data to fall back on if it is destroyed, damaged or doesn’t fit.
The good news is that this landscape is changing. Like those aerospace manufacturers, automakers, moldmakers and machine shops, dental practitioners are on their way to digitalization. Digital dentistry — is being recognized and accepted encompassing 3D scanning technology, dental CAD/CAM, CNC milling and now 3D printing — as the solution not just to the industry’s skills gap, but also to realizing greater accuracy and repeatability as well as better patient care. I recently spoke with Rik Jacobs, vice president, general manager of dental solutions at 3D Systems, about dentistry’s shift to digital and the role for 3D printing.
What Is Digital Dentistry?
Digital dentistry is an alternative to conventional, often manual dentistry procedures that relies on digital data rather than analog capture and manufacturing methods. It isn’t a single technology but rather a workflow, and one in which 3D printing is but the newest arrival. According to Jacobs, digital dentistry “starts at the chair,” with a 3D scan of the patient’s mouth, and includes the design software, materials, additive or subtractive equipment, and postprocessing, through to the final fitting.
Digital dentistry is not a single technology, but rather a workflow.
All of the steps in a digital dentistry workflow stand in contrast to those of conventional, analog dentistry. Conventional patient records include hand-drawn diagrams, traditional impressions and two dimensional X-rays. When three-dimensional information is needed for prosthodontics or orthodontics, an impression of the patient’s mouth is captured using trays of silicones or alginate. That impression is then poured with plaster to form a model. Frequently, that plaster model then becomes sacrificial tooling for molding or thermoforming the final device. If the resulting item is lost or broken, the process is not easily repeatable and must begin again with an impression.
By contrast, a digital dentistry workflow might still begin with an scannable impression or a model, but that model could be captured with a desktop scanner and converted into three-dimensional digital data. Or even better, that data could be gathered with an intraoral scan in a matter of minutes, without subjecting the patient to an uncomfortable tray of alginate. With a few additional processing steps via software, the data can be used for CNC milling or 3D printing a better-fitting device in the dental lab. If the patient later loses that device, the digital file can be easily called up and recreated.
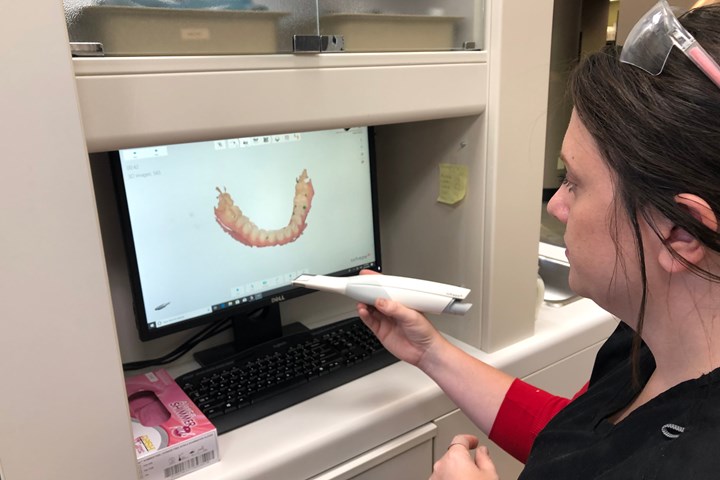
Handheld intraoral scanners like this one capture three-dimensional images of a patient’s mouth. Immediately digitalizing this information allows dental labs to design and mill or print dental devices much more rapidly. (More about this particular dental lab.)
The Digitalization of Dentures
As an illustration of how digitalization has and is changing the production of dental devices, consider dentures. Creating a set of dentures without a digital dentistry workflow requires a series of manual steps and five or more patient visits, Jacobs says. First, the doctor obtains an impression of the patient’s mouth, which is then cast in plaster. A technician applies wax to the plaster model and a bite plate to design the dentures using an articulator, and then creates a mold with additional plaster. The wax is melted out, and the mold can be injected with resin to form the denture. The device must then be broken out of the mold, cleaned and finished before fitting it into the patient’s mouth.
There are a number of challenges with this process, Jacobs says. First, the success of the device is entirely dependent on the accuracy of the impression; if this is off in some way, the dentures may be uncomfortable or require rework. In converting the impression to a plaster model, a mold and finally a resin device, air bubbles and shrinkage can cause similar problems with fit. The final dentures themselves will require polishing to achieve a smooth, comfortable finish — another manual step where fit can be compromised. Implicit in all of this is the skill of the dentists and technicians involved; the success of the process depends almost entirely on human involvement.
The introduction of CNC milling for dentures has been an improvement on this process. Scan data obtained from a plaster model or intraoral scan of the patient’s mouth can be used to create CAD/CAM files for this process. Cutting the device from a block or puck of material with G code reduces the manual work and increases the accuracy of the result, especially with a design based on intraoral scan data. And, files can be saved so that dentures can be cut again if needed.
Like molding, machining dentures from scan data based on a plaster model may introduce inaccuracies. Even if the machining code is based on an intraoral scan, milling dentures also poses some challenges. The machining process requires progressively finer burrs to achieve the smooth, glossy finish patients expect, which takes time. Dentures typically include features like undercuts that are challenging to mill, and may sometimes be impossible, which translates to a device that doesn’t fit as well as it should. The milling process also generates a significant amount of waste in excess material.
“When you think about milling one crown, that’s not much waste or time,” Jacobs says. “But for larger items like splints, retainers and dentures, the milling takes much more time. The size of the burr limits geometric freedom. And it’s not sustainable — there’s a lot of waste generated.”
Digital Dentistry with 3D Printing

Digital dentistry is progressing to the point that dedicated 3D printers are emerging, like the NextDent 5100. This resin-based 3D printer from 3D Systems can be used to make models, dental appliances, dentures and more. Photo: 3D Systems
CNC milling has made dentistry faster and more precise, but additive manufacturing will take it several steps further. When 3D printing is used as the manufacturing technology, scan data can be converted quickly into an STL or other print file, and sent directly to the machine. Direct digital manufacturing this way removes steps from the process, reduces the number of manual steps and patient visits, and enables dentists to deliver devices to patients much more quickly.
In the case of dentures, it is possible to directly 3D print the devices in resin without regard for the design difficulties like undercuts that might arise with milling. 3D printed dentures are faster and easier to produce, in addition to being more accurate, than conventional or milled dentures. And, they require little postprocessing. According to Jacobs, the printed surface is smooth enough that after a quick wash, it takes only about a minute with a mop or polish brush to create the final shiny gloss.
3D printing is still a relatively new technology within dentistry, but 3D Systems’ dental solutions team (and plenty of other equipment and material suppliers) sees future growth here.
“...3D printing is the technology to be productive and competitive in this market.”
“Ultimately for many applications we will use 3D printing because of freedom in geometry,” Jacobs says. “For dentures, surgical guides, models, orthodontic splints, retainers, I think that 3D printing is the technology to be productive and competitive in this market.”
Related Content
3D Printing as a New Product Launchpad
With 3D printing, Minnesota manufacturer Resolution Medical offers a fast, affordable route for individuals and small to medium-sized businesses to get new medical devices and other products off the ground and into the marketplace.
Read MoreNew Zeda Additive Manufacturing Factory in Ohio Will Serve Medical, Military and Aerospace Production
Site providing laser powder bed fusion as well as machining and other postprocessing will open in late 2023, and will employ over 100. Chief technology officer Greg Morris sees economic and personnel advantages of serving different markets from a single AM facility.
Read MoreIce 3D Printing of Sacrificial Structures as Small as Blood Vessels
Using water for sacrificial tooling, Carnegie Mellon researchers have created a microscale method for 3D printing intricate structures small enough to create vasculature in artificial tissue. The biomedical research potentially has implications for other microscale and microfluidics applications.
Read MoreZeda AM Production Plant in Ohio Now Open — Thoughts on the New Facility
73,000-square-foot metal powder bed fusion plant includes extensive machining capability plus separate operational models for serving medical versus other businesses.
Read MoreRead Next
Dental Lab Brings 3D Printing into Digital Dentistry Workflow
With 3D scan technology and resin-based 3D printers, Spectrum Dental Printing is changing the way dental devices are made — and potentially, how dentistry happens.
Read MoreInjection Mold or 3D Print? How Resolution Medical Pivots Production
Minnesota manufacturer Resolution Medical is finding opportunities for additive manufacturing via Carbon 3D printers as an alternative to injection molding for production.
Read MoreAt General Atomics, Do Unmanned Aerial Systems Reveal the Future of Aircraft Manufacturing?
The maker of the Predator and SkyGuardian remote aircraft can implement additive manufacturing more rapidly and widely than the makers of other types of planes. The role of 3D printing in current and future UAS components hints at how far AM can go to save cost and time in aircraft production and design.
Read More
.jpg;width=70;height=70;mode=crop)




















